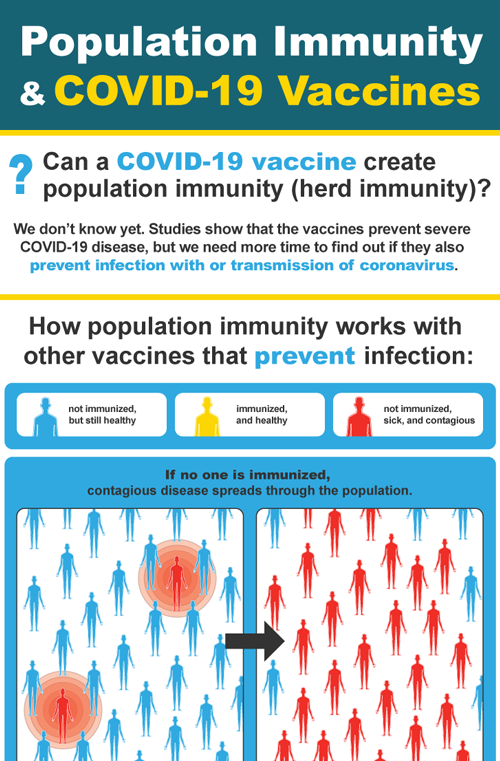
View the infographic: Population Immunity and COVID-19 Vaccines


The Science of COVID-19 Vaccines and Monoclonal Antibodies
What Are Vaccines?
A vaccine is a substance that teaches your body to recognize a foreign invader, such as a virus, sound an alarm to activate your immune system, and instruct your fighter cells and proteins to go to work to fight the virus. The goal of a vaccine is to eliminate or control the virus in your body, which could prevent infection, or control an infection from developing into disease. The vaccine causes the immune system to respond by looking as much like the invading virus as possible without causing disease itself.
Vaccines have been used for decades around the world. While smallpox is the only infectious disease to date that has been eliminated globally by vaccination, vaccines have reduced the burden of many other infectious diseases such as polio, measles, mumps, and pertussis. Most recently, vaccines for the prevention of human papillomavirus (HPV), pneumonia, and shingles have been developed.
COVID-19 Vaccines: How Did We Get Them So Fast
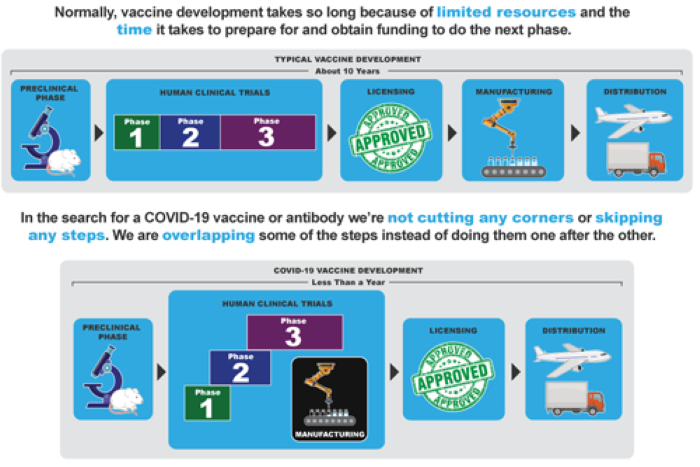
In the search for a COVID-19 vaccine or antibody we’re not cutting any corners or skipping any steps. We are overlapping some of the steps instead of doing them one after the other.
With funding from the U.S. government, these COVID-19 vaccines began getting manufactured in large quantities while the phase 3 trials were being conducted. This manufacturing was a risk, because we didn’t yet know if the vaccines were effective. This risk was taken because of the public health crisis. If the studies show the vaccines are not effective, they will be destroyed. At every stage of the vaccine development process our primary concern is the safety of the public.
View the infographic: COVID-19 Vaccines: How Did We Get Them So Fast?
Children, Youth and COVID-19 Vaccines

COVID-19 vaccines are now available for children 12 years and older!
View the infographic: Children, Youth and COVID-19 vaccines.
About Messenger RNA Vaccines

mRNA – Are they safe?
Long-term safety is still being studied, YES they are safe! Most side effects happen within 7 days of vaccination and last 1-3 days. More people reported side effects following the second dose. Read more about mRNA vaccines safety and side effects.

mRNA – How do they work?
mRNA vaccines give your body the information needed to defend against a virus. Read an overview of how mRNA vaccines work and the importance of receiving 2 doses.

mRNA – What are the benefits?
After receiving 2 doses, mRNA vaccines can reduce the risk of being hospitalized with severe COVID-19 disease and dying as a result of severe COVID-19 symptoms. Read more about the benefits and information on priority groups included in the vaccine trials, underscoring safety and efficacy for these groups.

mRNA – What do we still hope to find out?
There are many reasons why continued research for other COVID-19 vaccines is needed. Until we know more, we should continue wearing masks. Read more about what we hope to learn with more research.
What You Need To Know About The Johnson & Johnson (J&J)/Janssen Vaccine
The J&J/Janssen vaccine requires 1 dose to prevent COVID-19 disease, hospitalization, and death. Independent experts who reviewed the safety data have concluded that the vaccine is safe.
Population (Herd) Immunity and COVID-19 Vaccines
The studies have shown the COVID-19 vaccines are effective at preventing severe disease. This is important for the vaccinated people and their communities. It means people don't need so much time away from work or their families, and it means that the burden on hospitals and healthcare systems is reduced. We don't know yet if COVID-19 vaccines also prevent infection or prevent transmitting the virus to others. If people who are vaccinated can still get infected and transmit the virus to others, it will be harder to achieve population immunity.
We need the research to continue to help us find this answer.
What Are Monoclonal Antibodies?
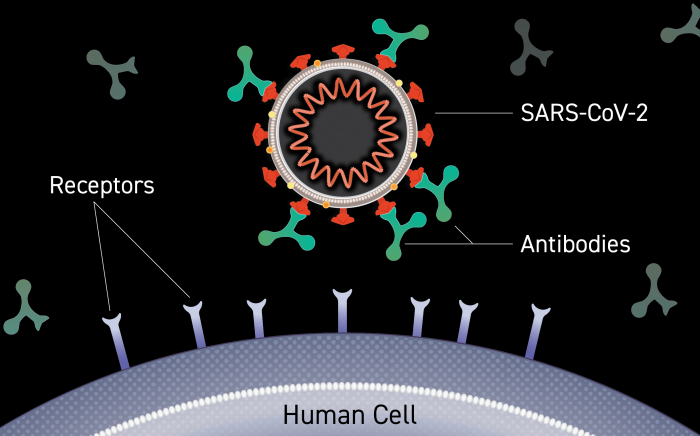
An antibody is a Y-shaped protein produced by B cells, which are part of the immune system. There are several different kinds of antibodies, and typically vaccines are designed to produce the antibodies that recognize and “tag” viruses as foreign invaders by binding to unique parts of a virus.
Antibodies that bind to the surface of a virus and block entry into a person’s cells can actually prevent infection or disease: this is called neutralization. These antibodies, which occur naturally in some people after vaccination or infection, can be copied in the lab and then given to people as a prevention option or treatment. The term “monoclonal” refers to these laboratory-made antibodies.
The development of monoclonal antibodies to prevent COVID-19 is important for a number of reasons, including:
- Monoclonal antibodies may be able to serve as another prevention option until a COVID-19 vaccine is available.
- Monoclonal antibodies may be able to provide immediate protection or treatment for those who are exposed and not yet vaccinated.
- Monoclonal antibodies may be required for people who cannot develop or maintain an adequate immune response after vaccination, such as older adults.
How Are Monoclonal Antibodies Different From Vaccines?
In traditional research, people get a vaccine and scientists wait to see if their bodies will respond to the vaccine by making antibodies against the virus. In antibody studies, we skip that step and give people the antibodies directly. We do this using intravenous infusions, commonly known as “getting an IV,” with shots into the skin or infusions under the skin. Another difference is that antibodies produced naturally by your body in response to a vaccine can last for a long time, but these laboratory-made monoclonal antibodies usually only last for a few months, thus requiring people to get multiple infusions or injections on a regular schedule.
Where Is the Latest Information on Coronavirus and COVID-19?
What we know about the coronavirus, SARS-CoV-2, and the disease, COVID-19, is constantly changing. To stay up to date on the most current information, we recommend that you visit the following websites for reliable and accurate information:
- US Epidemic
- Racial and Ethnic Disparities with COVID-19 in the US
- Global Epidemic
Information about how the epidemic is impacting the world (mathematical modeling):
- Johns Hopkins University
- IHME
Vaccine-Induced Seropositivity (VISP)
What Is VISP?
Antibodies help prevent infection. Most vaccines stimulate the body to make antibodies. If you get a COVID-19 vaccine, your body will likely develop antibodies to the virus. Because of this, some antibody-based tests for coronavirus infection may return a positive result even if you are not, or were not previously, infected with coronavirus. This is called a vaccine-induced seropositivity (VISP) test result.
Two Kinds of Tests Are Available for SARS-CoV-2
- A viral test tells you if you have a coronavirus infection. This test detects the presence of the actual coronavirus virus in your body. Some of these tests are referred to as PCR tests. A nasal swab or saliva sample is usually needed for this test.
- An antibody test tells you if you had a previous coronavirus infection. A sample of blood is needed to determine if your body has developed antibodies to the coronavirus.
Right now, VISP shouldn’t be a problem because the antibody tests that are widely used do not detect the type of antibody produced by the current COVID-19 vaccines being developed. Instead, they pick up on a different antibody produced by a natural infection with coronavirus. However, this could change in the future as new antibody tests are developed.
Vaccine Antibodies vs. Coronavirus Infection Antibodies
Your body will make different antibodies in response to coronavirus infection than in response to vaccination.
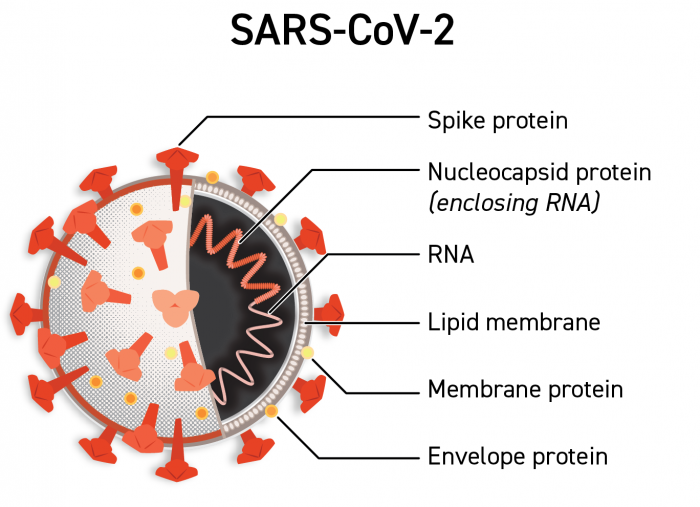
One of these antibodies is called a “spike antibody,” meaning that the antibody is directed at the spikes that surround the virus’s outer shell. The antibody attaches itself to the spikes on the virus in order to prevent the virus from attaching to your body’s healthy cells and causing infection. These are the types of antibodies that COVID-19 vaccines aim to teach your body to make in order to protect against infection.
Natural infection with coronavirus will produce different antibodies. These antibodies can bind to not just the spike, but also to other viral proteins such as the nucleocapsid. Current COVID-19 vaccines in development do not lead to antibodies against the nucleocapsid protein.
The antibody tests currently in use will only detect the second type of antibody that is produced by a natural infection with coronavirus. As time goes on and more vaccine candidates are tested, however, new antibody tests might be developed that also detect antibodies that binds to the virus’s spikes. If this happens, it means you could get a positive antibody test result, even if you have never had been infected with the coronavirus. Health care providers may not interpret your test results correctly as an immune response to a vaccine; they may incorrectly see it as an indication of prior infection with coronavirus. Once an effective vaccine is found and widely administered to the public, testing technology will need to clearly distinguish between vaccine responses and infection.
What Do I Do With This Information?
We have a few recommendations for anyone receiving a COVID-19 vaccine in a study:
- Be sure to ask for documentation from your vaccine study team that explains your participation in the study. It should include information about the SARS-CoV-2 “spike” vaccine, meaning that you may produce a spike antibody response.
- If you are asked to take a coronavirus antibody test (for example, as a condition of returning to work), be sure to specify that you need to have a “nucleocapsid” test done, and do not take any type of antibody test that might only be looking for spike antibodies.
- You can avoid this situation if you can get access to coronavirus viral testing (such as PCR), which detects the presence of the actual virus in your body. If possible, ask for this type of test and use the documentation of your vaccine study participation as your justification.
- We do not know if the COVID-19 vaccines being studied will lead to antibodies that can protect you from infection. We do not yet know if a positive antibody test means that you are less likely to get a coronavirus infection or COVID-19 illness.
Content last reviewed on July 15, 2021